The scale and tragedy of the U.S. opioid epidemic is unparalleled, with more than 100,000 overdose deaths occurring each year since 2021. The vast majority of drug overdose deaths are caused by a single source: fentanyl, an extremely powerful synthetic opioid.
But the latest data from the Centers for Disease Control and Prevention shows this brutal trend may have peaked. Since last fall, there has been a slight decline in overdose deaths overall, as well as a decline in overdose deaths from opioids, including fentanyl. But don’t celebrate yet. More than 102,000 deaths in the past 12 months are still well above pre-pandemic figures. For example, it’s estimated that more than 68,000 people died from overdoses each year from 2017 to 2019. The CDC says these recent figures are preliminary and may be underestimated.
It’s “clearly too early” to say deaths have peaked and will continue to decline, says Daniel Ciccarone, a professor of family and community medicine at the University of California, San Francisco, who studies the social, behavioral and medical aspects of the opioid epidemic. “We’ve had false peaks before.” Still, he says, “The number of deaths is still so high that it’s not optimistic, but there’s a lot of reason to think that things are getting better.”
Supporting science journalism
If you enjoyed this article, please support our award-winning journalism. Subscribe. By purchasing a subscription, you help ensure a future of influential stories about the discoveries and ideas shaping the world today.
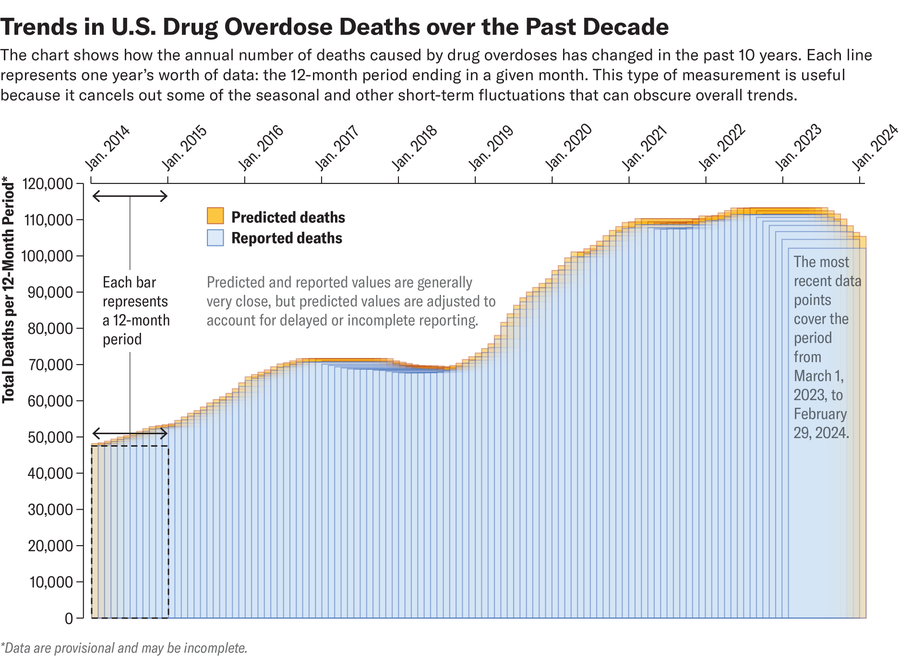
The reasons for the sudden increase in overdose deaths aren’t fully understood, but experts have a few theories.
One is that overdose deaths are starting to return to average levels seen before the COVID pandemic. Overdose deaths surged in the first few years of the pandemic. It’s not clear whether more people started using drugs or if death rates simply rose. The exact number of people using illicit drugs such as fentanyl is unknown. Increased stress and social isolation during the pandemic may have led some people to start using drugs or to use them more frequently or in more dangerous ways. Treatment for opioid use disorder was also disrupted, increasing the likelihood that if a person overdoses, there will be no one to intervene.
“The pandemic situation has improved a lot, and people are able to go out again, so they can socialize. They can get services. I think that part of the risk has been reduced, and I think that’s part of the reason for the decline,” said Magdalena Cerda, an epidemiologist and director of the Center for Opioid Epidemiology and Policy at the New York University Grossman School of Medicine.
Investments in treatment and intervention may be working to some extent, she adds. There has also been increased access to opioid use disorder medications such as buprenorphine and methadone, as well as the overdose-reversing drug naloxone (often referred to by the brand name Narcan), which is now available over the counter. Additionally, the availability of test strips and other types of drug-testing devices to detect fentanyl may have helped drug users avoid it, potentially preventing overdose deaths, Cerda says. This synthetic opioid is much more potent than other opioids and can cause an overdose at much lower concentrations.
A more dire explanation for these trends is that the population of people who were using fentanyl and at risk of overdose simply died out. If there aren’t enough susceptible people, the opioid epidemic will eventually die out on its own, like any other epidemic, Ciccarone says. An older generation with opioid use disorder is dying off, and younger generations are learning about the drugs’ deadly dangers and may be less willing to start using, adds Jay Yunick, assistant professor at the University of Maryland School of Social Work.
A reduced supply of fentanyl in some parts of the U.S. could also be a reason for the decline in overdoses. Most of the illegal fentanyl in the U.S. comes from Mexican drug cartels, which get their raw materials from China and other countries. The U.S. Drug Enforcement Administration has been cracking down on a Mexican cartel called the Sinaloa Cartel, which supplies fentanyl to much of the eastern U.S., and that could be contributing to the shortage, Ciccarone said. He’s heard similar fentanyl shortages reported in San Francisco recently. But because fentanyl is extremely cheap to produce and there’s no shortage of the raw materials it needs, Ciccarone said it’s unlikely that a supply shortage alone can explain the decline in deaths.
The national trends mask important regional differences: While overdose deaths are falling in most eastern U.S. states, many in the West are rising. Experts say when fentanyl was introduced to those regions may explain the differences. The eastern U.S., from the Midwest to the Appalachians, was first exposed to the drug around 2014, while the West Coast didn’t see much of it until 2019, Ciccarone said. “We joined the party late,” he said, adding, “It’s still a deadly party.”
Yunick agrees that the timing of fentanyl’s introduction is the most likely explanation for the East-West discrepancy: “It’s not really used here on the East Coast anymore, but it’s still found in some places on the West Coast,” he says. The fact that overdoses are starting to plateau or decline nationwide isn’t surprising, he says, but adds, “these numbers are unusually high.”
The demographics hardest hit by the U.S. opioid epidemic are also shifting: Fewer white people are dying from overdoses, while Black and Native American deaths are rising. High rates of homelessness and mental illness are also fueling the crisis, a sign of the compounding effects of income inequality.
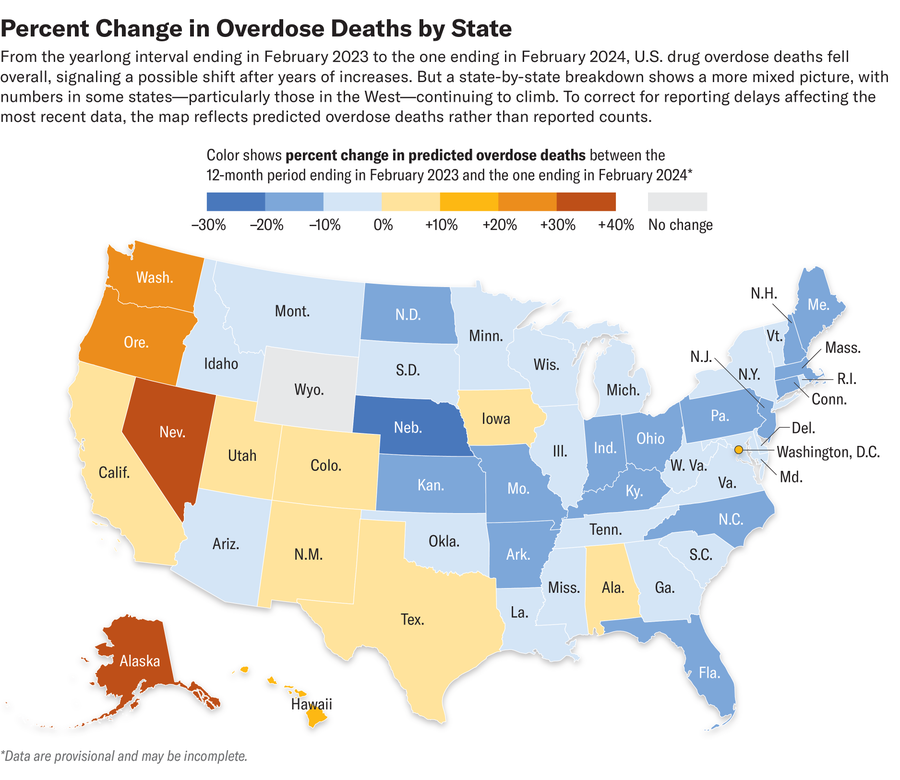
The rise in drug overdose deaths on the West Coast has led some states to take a tougher stance on visible drug use, even in places that previously relaxed penalties. In a landmark move in 2020, Oregon voted to decriminalize small amounts of certain drugs, including heroin, cocaine, and methamphetamine. However, under public pressure, the state recently reversed that policy. It is unlikely that decriminalizing drugs in Oregon led to an increase in opioid overdoses; this increase was also seen in California, Washington, and many other states that did not decriminalize.
“There’s not much evidence that it has had any effect other than the visibility of drug use,” Yunick said, “so the problem has become more visible and we’ve started to blame it on this law.”
While the number of deaths from opioid overdoses has fallen overall, the number of deaths from stimulants such as cocaine and methamphetamines has increased, although many of these are due to co-use with opioids. Contamination of other drugs with fentanyl has also been reported as a cause of accidental overdoses. Contamination can occur when mid-level distributors cut fentanyl and cocaine on the same surfaces or equipment without cleaning, but fentanyl shipped from Mexico is becoming increasingly pure, and some is shipped in finished pills. Also, people who use methamphetamine can be accidentally exposed to fentanyl by sharing smoking equipment. (Smoking fentanyl is on the rise in some areas.) But Ciccarone believes there is no evidence to support that this is happening on a large scale. Most people who use both fentanyl and methamphetamine are likely doing so intentionally, he says.
Experts are cautiously optimistic that overdose deaths are declining overall, but note there is still a long way to go to address the crisis. They call for expanded access to medications such as buprenorphine and methadone that can be used safely and effectively to wean people off illicit opioids. But the doses of these drugs needed to prevent withdrawal symptoms from fentanyl addiction may be higher than many insurance companies currently allow. Cerda and others argue that these limits should be raised to effectively treat more people. She also calls for making naloxone more affordable, expanding access to fentanyl test strips, and increasing investment in prevention programs for youth.
“We’re still at more than 100,000 overdose deaths per year, so that number is unacceptably high,” Cerda said, “but we are encouraged by the continued decline in overdose deaths over the past few months. We should continue to invest in the programs we know work to protect people from overdose deaths.”

